Did you know you can manage repeat prescriptions from Claremont Bank Surgery in the NHS App? Find out how to do it: www.nhs.uk/nhsapp

OR YOU CAN USE POD & POD ONLINE ...... See below for details
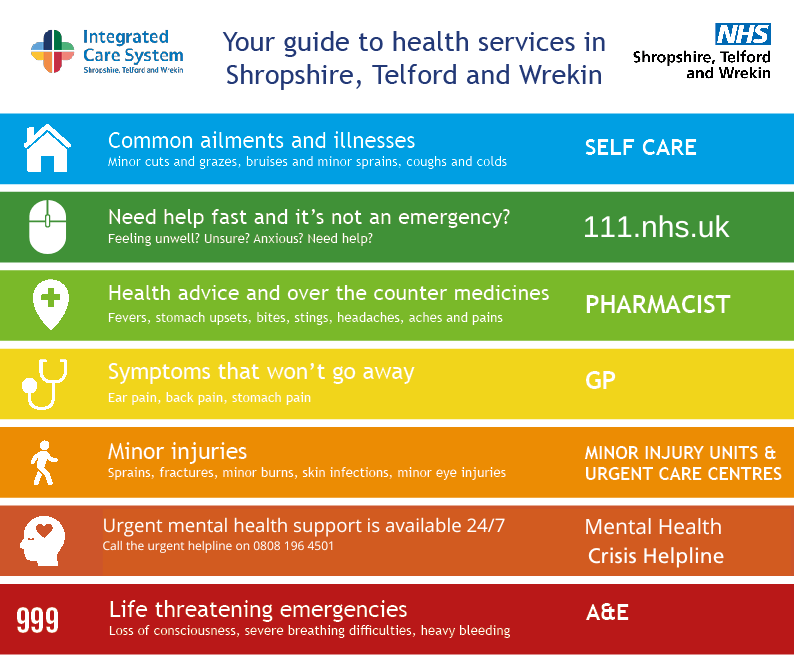
Quick guide to services
Important update on the Shrewsbury Health & Wellbeing Hub
Message sent on behalf of Dr Nick White, Chief Medical Officer at NHS Shropshire, Telford and Wrekin
As you may be aware from recent media reports, in January 2023 the national NHS (known as NHS England) issued a letter to NHS Shropshire, Telford and Wrekin which instructed that the national Cavell Centre Programme, and its constituent six pilot programmes, should be paused pending approval of the national business case.
At this point, the Programme Team for the Shrewsbury Health and Wellbeing Hub, the local name for the Cavell Centre Programme, took the decision to continue work on the site options appraisal, which was already underway, as we had contractual commitments with technical experts supporting the options appraisal work. We wanted to bring this phase of work to completion and await further instruction on the likely length of the pause.
We have previously shared our intention to hold a multi-stakeholder workshop to identify a preferred site option and prioritised site list. This would be the final site appraisal stage and on completion would be a key milestone to progressing to formal consultation later in the year.
Since January, we have received no further communication of when the business case will be going forward for approval. We are also aware that even if the business case did go forwards, there are still no guarantees that the capital funding would be made available in the current economic climate.
Given that indications now point to the pause being medium to long term, NHS Shropshire, Telford and Wrekin has reluctantly taken the decision to pause all further work and expenditure at this point. We will therefore not be holding the site options workshop that was originally planned and await further information from the national team.
It is important to clarify that this is a national directive for all six pilot programmes, and that the local projects as part of the Cavell Centre Programme cannot influence the decision.
Clearly, this is a hugely disappointing position given the significant amount of work that has been undertaken and the very clear case for change. NHS Shropshire, Telford and Wrekin and the Programme Team maintain its commitment to the project and to pursuing the right sustainable solution for General Practice in the South of Shrewsbury.
This does pose an extremely challenging situation to our practices if we are not able to access the £40-£60m national capital allocation for the programme. As has previously been shared, the case for changing how General Practice needs to be sustained over time has not altered.
At this point, there is no mechanism for securing this level of funding which means we now need to plan for an alternative future. As part of that, it is important to recognise that the uncertainty over the future of this development further emphasises the fragility of the status quo for the practices and their patients.
Our primary care estates strategy is currently under review, and we will need to consider the real prospect of not receiving this funding and addressing the current fragility of those respective practices.
As a health and care system we will do all we can to avoid practice closures, but we will need to consider the consequences of practices that may no longer be able to continue to provide services, and as a result hand back their contract. Our considerations will need to include how this will affect patients, staff and neighbouring practices should patient lists be dispersed.
To inform this thinking, we are now in discussions with the six practices about next steps and revisiting each practice individually to explore what could be achieved to support them going forward. However, it is important to note that this will be to stabilise the practices as best we can. It is not about futureproofing or sustaining them in the way that the development of the hub approach would have allowed given the very limited amount of capital funding that is available to NHS Shropshire, Telford and Wrekin.
We will keep you informed of any developments as and when we learn more.
Kind regards,
Dr Nick White
Chief Medical Officer
NHS Shropshire, Telford and Wrekin
Local NHS gets ready to ramp up lifesaving tests
Shropshire patients will soon benefit from quicker access to tests, checks and scans when a brand-new community diagnostic centre opens in Telford later this summer.
The government has approved the community diagnostic centre (CDC), one of four in the Midlands region, providing tests and treatments away from the acute hospitals.
Led by Shropshire, Telford and Wrekin Integrated Care System, the centre is set to transform how services such as MRI scans, ultrasounds, X-rays and blood tests are offered to local people.
Patricia Davies, Shropshire Community Health NHS Trust CEO, said: “This is really great news for residents, staff and services across the county – the centre will act as a one-stop shop offering a range of diagnostic checks, scan and tests to help reduce the backlog and diagnose patients more quickly.
“It will reduce waiting times for non-urgent tests and reduce the risk of cancellation, improving patient experience and outcomes, whilst at the same time bring additional capacity into our system to reduce pressure on other services.
“The plan is to provide even more services than we originally set out, including Echocardiograms, Lung Functioning Tests, Basic Sleep Studies, and Long COVID Clinics.
“We are working to a summer launch to give us enough time to put in place all the equipment, staff and training and make the necessary alterations to the building.”
Other services available in the new CDC include:
- CT (a series of X-ray images taken from different angles around the body)
- Non-Obstetric Ultrasound Scans (non-invasive scans)
- X-Ray
- ECG (Electrocardiograms)
- Phlebotomy (blood tests) with some on site point of care sample analysis.
The centre will be sited at Hollinswood House in Telford, which is currently undergoing a complete interior redesign to ensure it is fit for purpose and able to accommodate future demand.
NHS Shropshire, Telford and Wrekin supports charity to help make cervical cancer a thing of the past
Did you know…?
We are offering a new approach to improve access for patients to a same-day consultation with a healthcare professional. The aim is to direct patients to the most appropriate person to help them, which may be a GP or a community pharmacist.
From 1st July, if your symptoms can be resolved by a booked consultation with the community pharmacist instead of the GP, you will be given a same-day referral to a pharmacy of your choice. Your consultation may take place on the phone or in person at the pharmacy.
We think this is a good thing. We are working closely with your local pharmacist who is a highly trained and skilled clinician, experienced in treating minor illnesses. Once you see how great they are at helping with minor ailments we don’t think you’ll look back.
This will also help us to free up GP appointments for people with more complex health needs and ensure that everyone gets treated at the right time, by the right healthcare professional.
You can help us
We are keen to hear what you think and will be listening to your comments and feedback about your experience of using this new community pharmacist service.
.
.
.

.
...
.
HEALTHIER YOU - DIABETES INFORMATION AND ADVICE
For more information about Healthier You, please visit our website www.lwtcsupport.co.uk or For more information about how to reduce your risk of developing Type 2 diabetes, please visit www.diabetes.org.uk/preventing-type-2-diabetes


Children & Young People’s mental health in Shropshire, Telford & Wrekin
It has been widely reported over the recent months that Covid-19 has impacted the mental health of children and young people and this has led to a greater severity of need among many and an increased demand on services at a time when services have had to adapt to working under increased staff shortages.
However, the lack of ‘Tier 4’ beds (specialist inpatient beds for the most seriously unwell) in the county means that children and young people will be admitted to either Royal Shrewsbury Hospital or Princess Royal Hospital, or The Redwoods Centre (an adult mental health hospital) while waiting to be moved to a suitable hospital outside Shropshire.
Healthwatch Shropshire and Healthwatch Telford & Wrekin were asked to give these children and young people the opportunity to share their experiences and say what could have been done to improve the help they have received.
Lynn Cawley, Chief Officer of Healthwatch Shropshire, said, “The report highlights the need for the system to reduce waiting times and provide information, support and advice for children, young people and their families and schools while waiting for assessment, diagnosis and specialist services to prevent crisis. Alongside this there needs to be close monitoring to ensure children and young people can be prioritised according to need and closer partnership working to include schools and adult services to ensure no child or young person falls into the gaps between services. We heard from families and professionals who were calling for more awareness raising and training to help them to support the children and young people who are struggling.”
Barry Parnaby, Chair of Healthwatch Telford & Wrekin, said “Barry Parnaby, Chair of Healthwatch Telford & Wrekin, said “We have been aware of the pressure many children and young people are under - issues which have been exacerbated by the pandemic. This report provides a unique opportunity to understand and act to improve services based on the knowledge and experiences of young people, as well as their friends, family members and professionals within the sector.
“A key finding within the report centres on the need for additional support for young people and their families when using the services available. Whilst the report has now been completed, we look forward to continuing to work with local providers, users and others to improve services and support people where possible.”
Healthwatch is the independent health and social care champion. It gathers the views and experiences of patients, service users, carers, and the general public about services including hospitals, GPs, mental health services, community health services, pharmacists, opticians, residential care and children’s services. It also has statutory powers that it can use to influence service provision by encouraging improvements.
Claremont Bank Surgery – Face Mask Policy
Patients are required to wear a face covering/mask, use hand sanitiser, maintain social distancing and only enter the building only where necessary e.g. for an appointment, drop of a sample
The GP Practice is not the same as public transport, a restaurant or the supermarket – our visitors are unwell, vulnerable and may not be be vaccinated due to medical reasons.
We have experienced absence due to staff having Covid or close contact outside of work with someone who has Covid. In a practice with a small number of employees, this hugely affects our ability to answer the phone and provide appointments for you.
The continuing of appropriate infection control procedures protects our patients and their health and protects our staff to help you – without our staff we cannot deliver an effective, functioning service to you.
Our nurses and doctors have seen patients face to face for vital clinical procedures and specialist contraceptive procedures throughout the pandemic. It is worth noting that we are consulting with higher numbers of patients than we ever did before the pandemic, whilst also having played a big part in the vaccination programme delivery. Our doors have always been open.
We hope you will understand why we need to continue with these measures and keep the practice as safe for everyone as we can. We have all come so far in trying to minimise the impact of Covid, let’s continue to stay safe together.
IMPORTANT NOTE
If you attend the practice and refuse to wear a face covering without a valid exemption reason you may not be allowed access. The clinician who is due to see you has the right to ask you to rearrange your appointment.
Where you cannot wear a face covering due to a valid exemption we will need to make reasonable adjustments which may include rearranging your appointment to a different room, time and/or with a different clinician.